Go Live Faster with AI That’s Built for Healthcare
Explore Production-Ready AI Agents, Workflows, and Applications.
Book a DemoPurpose-built, pre-solved,
and ready to deploy from day one.
and ready to deploy from day one.
FEATURED SOLUTION
Care Management
Hear partnership StoryFEATURED SOLUTION
Appeals & Grievances
read case studyFEATURED SOLUTION
Prior Authorization
Read case studyPROVEN SOLUTIONS
Modernizing Healthcare’s Most Complex Workflows
Medical Prior Authorization
Ingest unstructured data from faxes and medical records, validate requests against dynamic clinical guidelines, and produce evidence-grounded determinations in seconds.
55%
reduction in
review time
review time
76%
auto-intake
approval rate
approval rate
18 min
saved per case, reclaiming up to 36,000 hrs/month
Care Management
Transform the traditionally reactive and resource-intensive care management process with intelligence that optimizes resource allocation and drives better health outcomes.
78%
REDUCTION IN
DOCUMENTATION TIME
DOCUMENTATION TIME
150K+
CARE PLANS GENERATED
ANNUALLY PER ENTERPRISE
ANNUALLY PER ENTERPRISE
Appeals & Grievances
Gather unstructured data from member correspondence and medical records, validate claims against dynamic payer policies and regulatory requirements, and automatically draft comprehensive, evidence-grounded response letters.
70%
CUT IN PREP EFFORT
PER CASE
PER CASE
93%
Accuracy in DOCUMENT
EXTRACTION
EXTRACTION
50%
FASTER TURNAROUND
ACROSS CASE TYPES
ACROSS CASE TYPES
Pharmacy Prior Authorization
Unify ingestion, normalization, clinical criteria evaluation, and real-time decision support into one governed agentic workflow.
98%
Accuracy in clinical
data abstraction
data abstraction
95%
Accuracy in clinical
contextualization
contextualization
90%
Auto-approval rate
Letters & Correspondence
Automate template creation and maintenance, with multilingual support and compliance alignment built in.
80%
reduction in templates and related IT requests
60%+
improvement in staff
productivity
productivity
40-60%
compliance risk
reduction
reduction
Payment Integrity
Embed AI-led intelligence upstream, across both provider submission and health plan pre-payment review, before improper claims are ever paid.
40-60%
improved productivity
0.5-4%
recoverable leakage
Claims Processing
Structure and validate claim attachments and notes at intake. Enforce policy rules, boost accuracy, and reduce downstream appeals.
55%
reduction in adjudication cycle time
40-60%
improved productivity
20-40%
improved Auto-adjudication rates
Risk Adjustment
Proactively detect missed conditions, validate documentation, and surface coding opportunities before they slip through.
20%
increase in verified and
supported RAF yield
supported RAF yield
50%
reduction in manual
chart review
chart review
50%
decrease in retrospective
vendor spend
vendor spend
Eligibility Verification
Consolidate plan data across systems to deliver instant answers on coverage and cost for members and providers alike.
2.5M
cases handled across
all lines of business
all lines of business
85k+
requests processed
per month at scale
per month at scale
60%
extraction accuracy for
HEDIS measures
HEDIS measures
Complex Document Processing
This solution uses Compound AI to categorize, structure, and route documents rapidly and accurately.
98%
accuracy in clinical
data abstraction
data abstraction
93%
precision in
document extraction
document extraction
80%
manual workload
reduction
reduction
Intake, Extraction, and Case Creation
Convert unstructured inputs into structured, actionable cases, eliminating redundant steps.
94%
fully automated
intake
intake
98%
accuracy in clinical
data abstraction
data abstraction
93%
precision in
document extraction
document extraction
See a Solution in Action
Let our team walk through how we transform complexity with living intelligence.
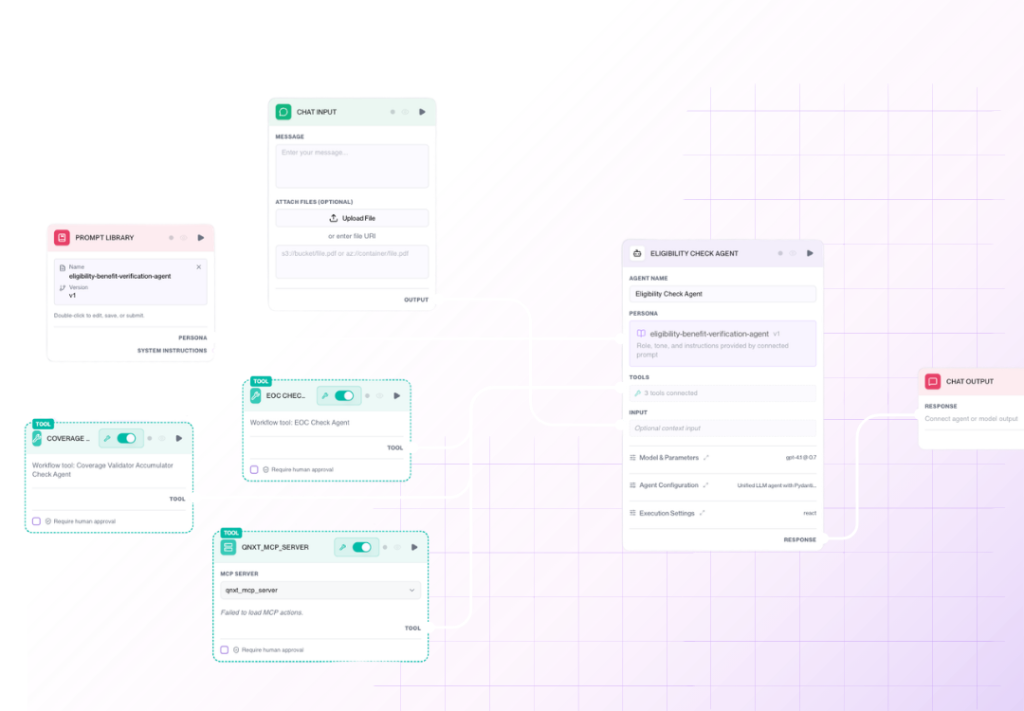
Don’t settle for incremental automation.
Move faster, make better decisions, and operationalize AI across the workflows that matter most.